The “Exercise for Aging” That Physical Therapists Wish Every Senior Knew (But Few Do)

Every year, 1 in 4 adults over age 65 will fall. Most of them were never told about the one exercise that could have stopped it.
You might be walking daily. Maybe doing some light stretching. That feels like enough. But underneath the surface, your muscles are quietly shrinking — and walking alone cannot fix that.
Physical therapists see this gap every single day. Seniors come in after a fall, after a fracture, after losing the ability to get up from a chair. And almost every time, the same tool could have helped them before things got bad.
This article will show you what that tool is, why it works, what the science says, and exactly how to start — today, at home, with no gym required.
‘You can see the exercises starting from point number 6’
Point One: The Silent Crisis Stealing Seniors’ Independence
Most people do not feel muscle loss happening. That is what makes it dangerous.
It starts at age 30. Your body begins losing 3 to 5 percent of muscle mass every decade. You do not notice it. Life goes on. Then you hit 60, and things start to change faster.

After age 50, muscle mass drops 1 to 2 percent every single year. Strength declines even faster — about 3 percent per year after age 60.
By the time you struggle to rise from a chair or carry groceries, the loss has been going on for decades.
This condition has a name: sarcopenia. It affects 5 to 13 percent of adults aged 60 to 70. By age 80, up to 50 percent of people have it. In the United States alone, sarcopenia-related care cost an estimated $18.5 billion — and that number is from the year 2000.
The real cost is personal. It is the loss of independence. The fear of falling. The feeling that your body is no longer reliable.
The good news? You can slow it down. You can even push back.
3 Tips:
- Do not wait for a fall to take muscle loss seriously
- Ask your doctor to check your grip strength and walking speed — these are early warning signs
- Know that sarcopenia is not inevitable — it responds directly to the right exercise
Point Two: Why Walking Alone Is Not Enough

Walking is good for you. This is not a debate. It helps your heart, your mood, and your blood pressure.
But here is what walking cannot do: it cannot stop your muscles from shrinking.
Walking is a low-resistance activity. Your muscles are not being challenged enough to grow or even hold their current size. You are moving, but the muscles are not getting the signal to stay strong.
The World Health Organization says adults over 65 need at least 150 minutes of moderate aerobic activity per week. But it also says they need muscle-strengthening exercises on 2 or more days per week. Most seniors only do the first part.
A 2025 review published in the International Journal of General Medicine confirmed that aerobic exercise like walking helps the heart and lungs. But cardio alone does not improve the neuromuscular coordination that keeps you from falling.
Walking cannot rebuild what sarcopenia takes away. It cannot retrain your balance system. And it cannot stop the quiet loss of strength that leads to fractures, falls, and loss of independence.
You need something more.
3 Tips:
- Keep walking — but add strength work on 2 separate days each week
- If walking is your only exercise, you are doing half the job
- Think of cardio and resistance training as a team, not a choice
Point Three: The Exercise Physical Therapists Actually Prescribe Most

Physical therapists have a go-to tool. It is not yoga. It is not water aerobics. It is progressive resistance training.
That might sound intimidating. It is not. This is not bodybuilding. It is not lifting heavy weights until you collapse. It is simply making your muscles work against some form of resistance — your own body weight, a resistance band, or light weights — and doing it regularly.
PTs prescribe it because it directly fights sarcopenia. It builds back what age takes away. It improves balance, bone density, and the neuromuscular system — the connection between your brain and your muscles.
A 2025 study confirmed that regular resistance training can increase muscle strength by up to 25 percent in seniors. That is not a small number. That is the difference between needing help to get off the couch and doing it on your own.
NIH aging expert Dr. Rosaly Correa-de-Araujo put it simply: “You need to have resistance training because this is going to help build your strength.”
The National Strength and Conditioning Association recommends 2 to 3 sessions per week. That is it. Two days a week can change your life.
3 Tips:
- Resistance bands are the best starting tool — cheap, safe, and easy to use at home
- Start with just 2 sessions per week and build from there
- You do not need a gym — a chair and a band are enough to begin
Point Four: How Resistance Training Stops Falls Before They Happen

Falls are not just scary. They are deadly. They are the leading cause of injury-related hospitalization for older adults worldwide.
One in 4 people aged 65 and older will fall this year. Many will never fully recover.
Your balance system depends on three things working together: your eyes, your inner ear, and the sensory nerves in your muscles and joints. All three of these weaken with age. When one fails, the others have to pick up the slack. When all three are weak, a small stumble becomes a serious fall.
Resistance training directly strengthens the muscular part of this system. It also improves proprioception — your body’s ability to sense where it is in space. That is what stops you from tripping on a curb or losing your footing on wet pavement.
A 2025 meta-analysis confirmed that resistance exercise improves lower limb strength, balance, flexibility, and coordination in older adults. It also builds psychological confidence — seniors who train feel less afraid of falling, and that confidence keeps them active.
People with sarcopenia are nearly twice as likely to be hospitalized as those without it. Resistance training is how you change those odds.
3 Tips:
- Practice single-leg standing daily — even 10 seconds per side helps retrain balance
- Focus on leg and glute strength — these muscles protect you most during a stumble
- A physical therapist can assess your specific fall risk and build a targeted plan
Point Five: The Brain Bonus Nobody Talks About
Most people think resistance training is only about muscles. They are wrong.
Your muscles and your brain are in constant conversation. When you do resistance training, you are not just strengthening your body. You are sending signals that help your brain stay sharp.
Research covering studies from 1970 to 2025 found strong evidence that resistance training improves memory, attention, and mental flexibility in older adults. These are not small gains. These are the skills that keep you independent — remembering medications, making decisions, staying organized.
When muscles work hard, they release chemicals called myokines. These travel through the bloodstream and reach the brain, where they support the growth of new brain cells and protect existing ones.
Neuroimaging studies show that resistance training can actually increase the thickness of brain tissue in the hippocampus — the part that handles memory — and the prefrontal cortex, which controls decision-making.
A 2025 JAMA Network Open study found that people who stayed physically active in midlife and later life had more than a 40 percent lower risk of developing dementia.
You are not just protecting your body when you lift. You are protecting your mind.
3 Tips:
- Combine resistance training with learning something new — the brain benefits double
- Consistency matters more than intensity for brain health — twice a week, every week
- Do not skip sessions after age 70 — this is when brain protection matters most
Point Six: Five PT-Approved Exercises Seniors Can Start Today

You do not need a gym. You do not need a trainer. You need a chair, some floor space, and about 20 minutes.
These five exercises come directly from what physical therapists use with their senior patients. Each one targets a specific weakness that leads to falls, loss of independence, or daily pain. They are safe. They are proven. And you can do every single one at home, starting today.
Start with 2 sets of 10 repetitions for each exercise. Do this routine twice a week. Rest at least one day between sessions.
Exercise 1: The Chair Stand — Build the Strength to Get Up on Your Own

What It Is: Sit on the edge of a chair. Place your feet flat on the floor, hip-width apart. Cross your arms over your chest or stretch them straight in front of you. Then slowly push yourself up to standing. Pause at the top for one second. Slowly lower back down. That is one repetition.
Why It Matters: This single movement targets your quadriceps — the large muscles along the front of your thighs. These muscles are responsible for almost every functional movement you do each day. Standing up from a toilet. Getting out of a car. Rising from a couch. When your quads are weak, every one of these tasks becomes harder and riskier.
Research from Brown University Health confirms that strengthening the quadriceps directly reduces both fall risk and mortality in older adults. That is a big claim. But it is backed by evidence.
Many seniors use their hands to push off the chair arms. That is a sign your quads need work. The goal is to eventually rise without using your hands at all.
How to Make It Easier: Place a firm pillow on the seat to raise the height. A higher seat means less distance to travel and less force needed.
How to Make It Harder: Slow down the lowering phase. Take 3 full seconds to sit back down. This “slow negative” builds more muscle than the upward push alone.
Target Muscles: Quadriceps, glutes, core
3 Tips:
- Keep your chest up and your weight in your heels as you rise — leaning forward too much puts strain on your knees
- If you feel shaky, keep the chair against a wall so it cannot slide
- Aim for 10 reps per set — if 10 feels easy after 3 weeks, do 12
Exercise 2: Calf Raises — Fix Your Walking Stability in 5 Minutes a Day
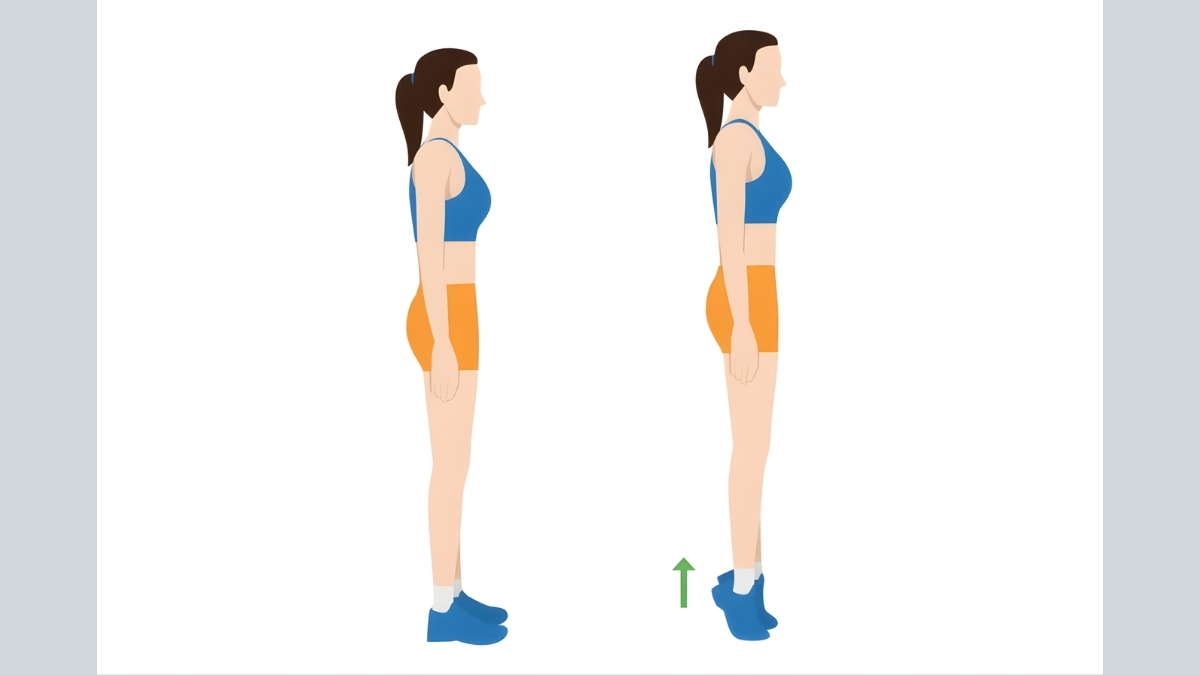
What It Is: Stand behind a sturdy chair. Hold the back of it lightly for balance — do not lean on it. Place your feet flat, hip-width apart. Slowly rise up onto your toes as high as you comfortably can. Hold for one second at the top. Then slowly lower your heels back to the floor. That is one repetition.
Why It Matters: Most people ignore their calves. Physical therapists do not. Your calf muscles do far more than most people realize. They push you forward when you walk. They absorb impact when you land a step. They stabilize your ankle when the ground is uneven — a wet sidewalk, a grassy yard, a sloped driveway.
Brown University Health physical therapists specifically recommend calf raises because stronger calves improve walking speed and dramatically lower fall risk on uneven surfaces.
Weak calves also lead to poor circulation in the lower legs, which causes swelling, fatigue, and cramping. Regular calf raises help pump blood back up toward the heart.
How to Make It Easier: Do this seated. Sit in a chair with feet flat and simply lift your heels off the floor while keeping your toes down. It is less intense but still effective.
How to Make It Harder: Do one leg at a time. Stand on one foot and perform the raise. This significantly increases the balance and strength demand.
Target Muscles: Gastrocnemius (upper calf), soleus (lower calf), ankle stabilizers
3 Tips:
- Go slow on the way down — the lowering phase is where the real strengthening happens
- Do not bounce at the bottom — full range of motion means heels fully down between reps
- If you have plantar fasciitis or ankle pain, do the seated version and check with your doctor first
Exercise 3: Single-Leg Balance — Retrain the System That Stops You From Falling
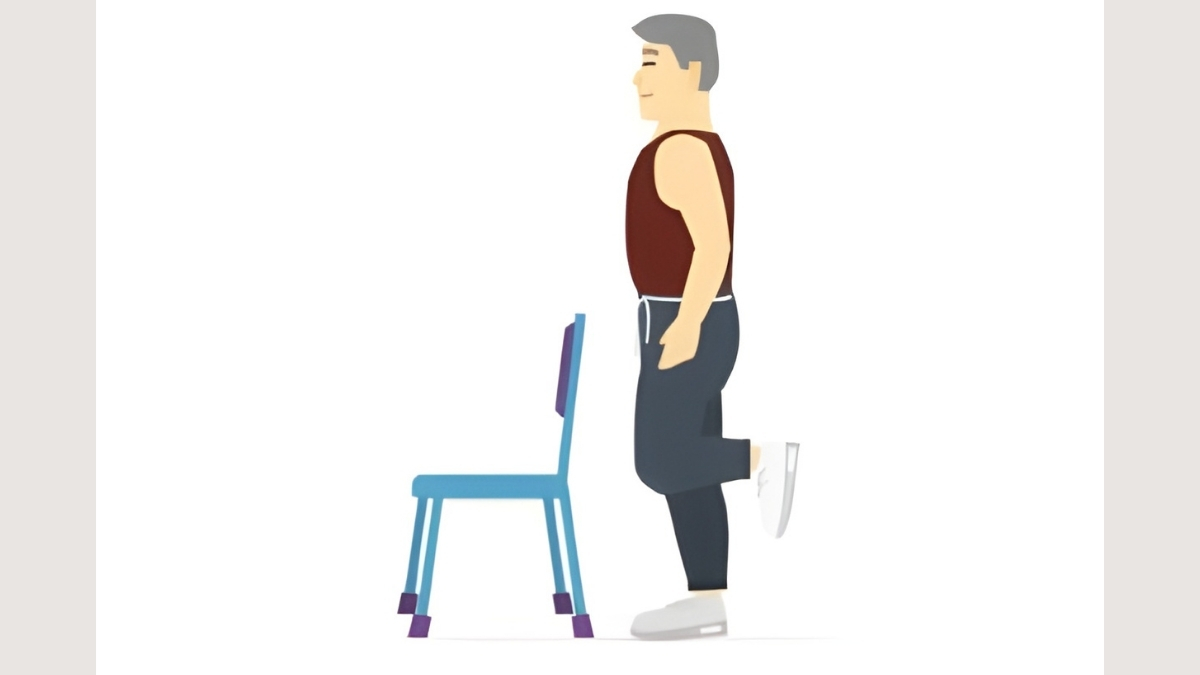
What It Is: Stand behind a chair and hold the back lightly with one hand. Lift one foot a few inches off the floor. Stand on the other leg. Hold for 10 seconds. Switch feet. That is one set. Work up to 30 seconds per side over time.
Why It Matters: This exercise looks simple. It is one of the most important things a senior can do.
Your ability to balance depends on three systems: your vision, your inner ear, and the sensory nerves in your muscles and joints. All three weaken with age. Single-leg balance training directly stimulates those nerves and teaches them to respond faster.
This is called proprioception — your body’s ability to sense where it is in space. It is what catches you when you stumble. When proprioception is poor, a small trip on a rug becomes a broken hip.
Physical therapists at Oasis Therapy Midwest explain that exercises targeting sensory feedback pathways — like single-leg standing — help the nervous system adapt and improve its response to sudden balance challenges.
You do not need equipment. You do not need much space. You need 2 minutes and consistency.
How to Make It Easier: Keep both hands on the chair back and just shift most of your weight to one leg without fully lifting the other foot.
How to Make It Harder: Let go of the chair completely. Then try it with your eyes closed for 5 seconds — this removes visual input and forces your other balance systems to work harder.
Target Muscles: Tibialis anterior, peroneals, hip stabilizers, core
3 Tips:
- Do this near a wall or sturdy surface every time — safety first, always
- Practice daily, not just on workout days — even 30 seconds per side at the kitchen counter counts
- If you wobble a lot, that is normal at first — wobbling means your nervous system is working and learning
Exercise 4: Resistance Band Rows — Fix Your Posture and Protect Your Spine

What It Is: Sit in a sturdy chair. Loop a resistance band around something fixed at waist height — a door handle, a stair railing, or a bedpost. Hold one end of the band in each hand. Start with your arms extended straight in front of you.
Pull both hands back toward your waist, squeezing your shoulder blades together. Hold for one second. Slowly return to the start position. That is one repetition.
Why It Matters: Most seniors have weak upper backs. This happens from years of sitting, looking down at phones, and doing little overhead or pulling work. Weak upper back muscles cause the classic “forward hunch” that shifts your center of gravity forward — which is a major cause of falls.
Resistance band rows directly target the muscles between your shoulder blades. These muscles pull your shoulders back and keep your spine upright. Better posture means a better center of gravity. A better center of gravity means fewer falls.
Senior Fit Now notes that resistance bands are ideal for older adults because the resistance is adjustable and the movement is joint-friendly. Unlike dumbbells, bands do not put sudden stress on your wrists, elbows, or shoulders.
How to Make It Easier: Use a lighter band (usually yellow or green). Shorten the distance you pull — even a small range of motion still works the muscles.
How to Make It Harder: Use a heavier band (blue or black). Pause for 3 seconds at the end of the pull before releasing.
Target Muscles: Rhomboids, middle trapezius, rear deltoids, biceps
3 Tips:
- Keep your elbows close to your sides as you pull — flaring them out changes the muscles being worked
- Do not lean back during the pull — keep your back straight and let your arms do the work
- If you do not have a resistance band, use a folded towel looped around a door handle — it works the same way
Exercise 5: Glute Bridge — The Floor Exercise That Rebuilds Your Foundation

What It Is: Lie flat on your back on a firm surface — a yoga mat or carpet works well. Bend your knees and place your feet flat on the floor, about hip-width apart. Keep your arms flat at your sides.
Press your feet into the floor and slowly lift your hips up until your body forms a straight line from your shoulders to your knees. Hold for 2 seconds at the top. Slowly lower your hips back down. That is one repetition.
Why It Matters: Your glutes are the largest and most powerful muscles in your body. They control nearly every lower-body movement — walking, climbing stairs, standing up from the floor, and recovering from a stumble.
When glutes are weak, your lower back compensates. That leads to chronic back pain. It also leads to poor walking mechanics, which increases fall risk.
The glute bridge is one of the few exercises that strengthens the glutes without putting pressure on your knees or hip joints. This makes it ideal for seniors with arthritis or post-surgical limitations.
Physical therapists prioritize glute bridges because they also strengthen the hamstrings and the lumbar stabilizers — the deep muscles along your lower spine that keep you upright all day.
How to Make It Easier: Do not lift as high. Even a small hip raise off the floor still activates the glutes. Use your hands to push lightly on your thighs for a little help at first.
How to Make It Harder: Hold the top position for 5 seconds instead of 2. Or try a single-leg version — extend one leg straight while bridging on the other.
Target Muscles: Gluteus maximus, hamstrings, lumbar erectors, core
3 Tips:
- Press through your heels, not your toes — this keeps the focus on the glutes rather than the quads
- Do not arch your lower back at the top — your hips should align with your knees and shoulders
- If getting down to the floor is difficult, ask a family member to help the first time — getting back up is part of the exercise
Point Seven: How to Start Safely and What to Avoid

Starting is the most important step. But starting wrong can set you back.
Before you begin any new exercise program, talk to your doctor. This is especially true if you have arthritis, osteoporosis, heart conditions, or if you have had recent surgery. A physical therapist can run a full assessment and design a plan built for your exact situation.
Start slow. Two sessions per week is enough. Research shows older adults need at least 16 weeks of consistent training to see real muscle changes — because protein synthesis slows with age. Be patient. The results are real, but they take time.
Never ignore sharp joint pain. Muscle burn is normal. Sharp or stabbing pain is not. Stop immediately if you feel chest tightness, dizziness, or shortness of breath.
Progress matters too. Your nervous system adapts. If you keep doing the same thing forever, you stop improving. Every few weeks, add one more repetition, or use a slightly stronger resistance band.
If getting to a clinic is hard, telehealth physical therapy is now widely available. Many Medicare plans in 2026 cover in-home physical therapy visits — check your coverage before assuming you have to pay out of pocket.
3 Tips:
- Never skip the warm-up — 5 minutes of easy walking before resistance work protects your joints
- Track your reps in a simple notebook — progress feels real when you can see it
- If pain lasts more than 24 hours after a session, reduce intensity and check with your PT
Point Eight: Resources, Tools, and Where to Get Real Help in 2026

You do not have to figure this out alone. Good help is available — and much of it is free.
Find a physical therapist: Go to ChoosePT.com, run by the American Physical Therapy Association. You can search by location and filter by specialty, including geriatrics. This is the most reliable way to find a licensed PT near you.
Free exercise program: AARP offers the Couch-to-Fit Challenge — 30 days of fitness videos, each under 15 minutes, designed specifically for older adults.
Free reading: The NIH published “Slowing Sarcopenia” in April 2025 at newsinhealth.nih.gov. It is written in plain language and covers everything from resistance training to protein intake.
Fall prevention resources: The National Council on Aging at ncoa.org has community programs and free tools focused entirely on fall prevention for seniors.
Beginner exercise guides: SeniorFitNow.com offers step-by-step exercise breakdowns written for adults over 65.
Equipment to start: A basic set of resistance bands costs $10 to $20 online. A foam balance pad costs around $15. These two items are enough to run a complete home program.
In 2026, Medicare has expanded in-home physical therapy coverage. Many plans now cover home visits specifically for aging-in-place care. Call your plan and ask directly.
3 Tips:
- Start with ChoosePT.com before buying any equipment or program
- Use the AARP free challenge to build the habit before adding more intensity
- Check your Medicare plan — you may already be covered for in-home PT visits
Lastly,

Progressive resistance training is the most proven, most recommended, and most ignored exercise for aging adults. It fights muscle loss. It cuts fall risk. It protects your brain. And it takes only two sessions per week to work.
Pick one exercise from Point Six. Do it today. Then talk to your doctor this week.
The best exercise for aging is the one you start. Physical therapists agree — resistance training is where to begin.
Physical therapists reveal the #1 exercise seniors need to stop falls, build strength, and stay independent. Start today — no gym required.






