Nearly 50% of U.S. Adults Now Have Cardiovascular Disease, AHA Warns.

If you’re sitting in a room with 10 people right now, statistically, five of them — possibly including you — already have some form of cardiovascular disease.
That’s not a scare tactic. That’s what the American Heart Association’s latest data actually shows.
Most people have seen the headlines. But they don’t know what “cardiovascular disease” really includes, whether they’re personally at risk, or what they can realistically do about it today.
This article breaks down the AHA’s 2025 and 2026 data in plain language. You’ll learn which risk factors affect you most, which ones you can actually control, and exactly what steps to take to protect your heart in 2026. No medical jargon.
No overwhelming lists. Just clear, honest information you can act on.
This article is structured into 7 Sections—read them one by one to understand why cardiovascular disease is rising among U.S. adults and what it means for
prevention and long-term heart health.
Section 1: What the AHA’s Latest Data Actually Says About Heart Disease in America
The numbers are serious. And most people don’t know how serious.
The AHA’s 2025 statistical update confirmed that cardiovascular diseases now kill more Americans than all forms of cancer and accidental deaths combined. In 2022 alone, 941,652 people died from cardiovascular disease. That’s roughly 2,500 deaths every single day.
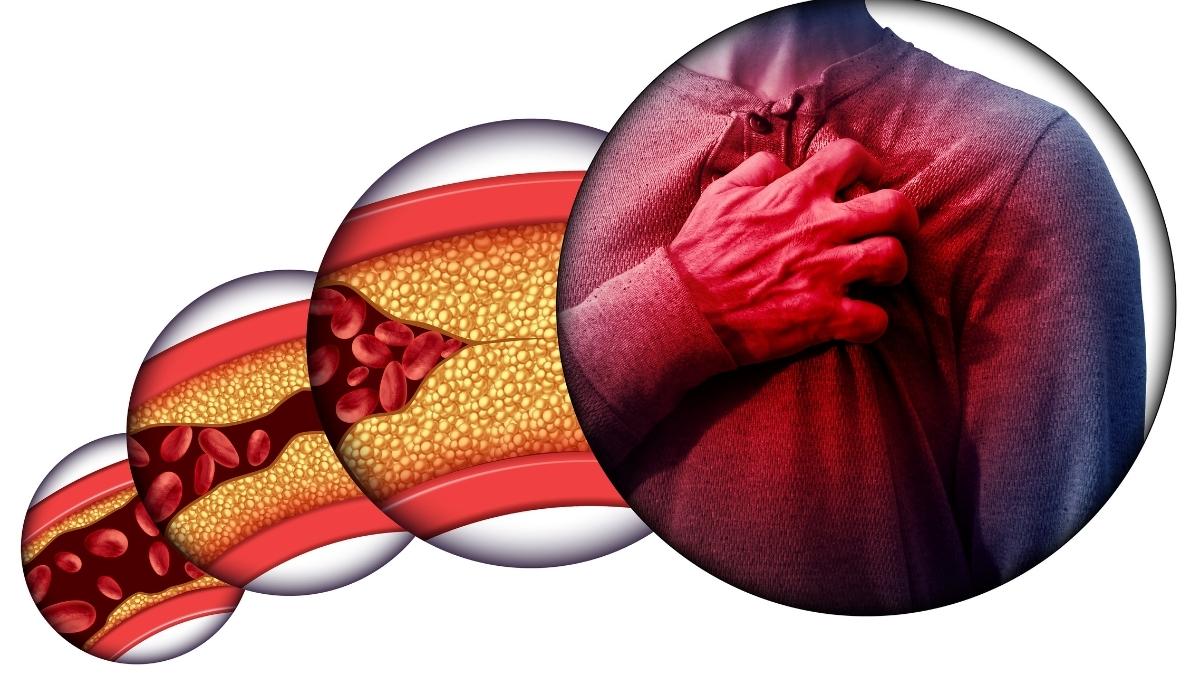
And the numbers are climbing. That 2022 figure was more than 10,000 higher than the year before.
The cost is rising too. Direct cardiovascular care costs jumped from $189.7 billion in 2012–2013 to $233.3 billion in 2020–2021. By 2050, experts project a 300% increase in related healthcare costs.
There’s also a newer concern. The AHA’s 2026 update introduced an entirely new chapter on cardiovascular-kidney-metabolic (CKM) syndrome — a condition that links heart disease, chronic kidney disease, diabetes, and obesity together. It already affects nearly half of all U.S. adults.
This isn’t just a heart problem anymore. It’s a whole-body crisis — and it’s affecting people who feel perfectly fine.
Section 2: Who Is Most at Risk and Why These Numbers Keep Getting Worse
The risk is not spread equally. And knowing where you fall matters.

Black women carry the highest rates of obesity (57.9%) and high blood pressure (58.4%) of any group in the U.S. Hispanic men have the highest rate of diabetes at 14.5%. These aren’t small differences — they represent real, measurable gaps in who gets sick and who gets help.
High blood pressure is now the most widespread risk factor. It affects 1 in 2 U.S. adults. But only 23.4% of those being treated actually have their blood pressure under control. That gap is dangerous.
Hypertension-related death rates have nearly doubled in the last two decades — from 23 per 100,000 in 2000 to 43 per 100,000 in 2019. Middle-aged adults aged 35–64 have been hit the hardest.
Obesity has now surpassed smoking as a leading health threat. Excess weight is linked to 1,300 deaths per day and cuts life expectancy by up to 2.4 years. Even more alarming — up to 40% of U.S. children now carry an unhealthy BMI.
Section 3: The Five Risk Factors You Can Actually Do Something About

Here’s the part that matters most. Most of the biggest risk factors are within your control.
A study covering more than 2 million people worldwide found something remarkable. Men and women who had none of five key risk factors at age 50 lived more than a decade longer than those who had all five. Women gained up to 14.5 extra years free of cardiovascular disease.
Those five modifiable factors are: high blood pressure, abnormal BMI, high non-HDL cholesterol, smoking, and poor blood sugar control.
Quitting tobacco works fast. Heart disease risk starts dropping within just one day of quitting. After one full year without cigarettes, your heart disease risk drops to roughly half that of someone who still smokes.
The AHA’s Life’s Essential 8 framework covers all the key areas — physical activity, healthy diet, healthy body weight, sleep health, cholesterol, blood pressure, blood sugar, and not smoking.
As Dr. Keith Churchwell of Yale School of Medicine said plainly: “Too many people are dying from heart disease and from stroke.” The factors causing those deaths are largely preventable.
Section 4: Heart-Healthy Eating in 2026 — What the Latest Guidelines Actually Say

Food is one of the most powerful tools you have. And the 2025–2030 Dietary Guidelines for Americans are clearer than ever.
The guidelines push hard on one thing: eat real food. Cut added sugars, refined grains, and highly processed products. Add more fruits, vegetables, whole grains, healthy fats, and lean proteins.
This matters because approximately 45% of cardiometabolic deaths — from heart disease, stroke, and diabetes — are directly linked to poor diet. And 70% of U.S. adults currently carry excess weight or obesity.
Two eating patterns stand out in clinical research. The Mediterranean diet is associated with reduced cardiovascular mortality. The DASH diet is associated with lower risk of coronary artery disease. Both work. Both are practical.
Simple targets to aim for: keep saturated fat under 10% of daily calories. Use olive oil as your main fat. Limit sodium to under 2,300 mg per day. Aim for 8–10 servings of fruits and vegetables daily.
Free resources to use: the NHLBI DASH diet guide and the AHA’s Heart-Check Certification program at heart.org.
Section 5: Exercise, Sleep, and Daily Habits That Protect Your Heart Long-Term

You don’t need to run marathons. You need consistent, moderate movement — and good sleep.
The AHA recommends at least 150 minutes of moderate-intensity aerobic activity per week. That’s 30 minutes, five days a week. A brisk walk counts. So does cycling, swimming, or dancing.
The research behind this is strong. Two large studies found that people who combined regular activity, good nutrition, healthy weight, and not smoking reduced their cardiovascular disease risk by more than 80% and their diabetes risk by more than 90%.
Sleep is now part of the AHA’s Life’s Essential 8. Poor sleep raises blood pressure and increases inflammation markers throughout your body. Aim for 7–9 hours per night consistently.
Stress matters too. Chronic stress keeps cortisol and blood pressure elevated for long periods, which damages the heart over time. Managing stress isn’t optional — it’s cardiac protection.
Tools to help: use Apple Health or MyFitnessPal to track daily activity. Use the AHA’s Life’s Essential 8 self-assessment at heart.org to see exactly where you stand.
Section 6: Screenings and Tests Every Adult Should Get in 2026

You can’t manage what you don’t measure. These are the tests that matter most.
Essential Screenings
Blood Pressure
Get checked at least every two years starting at age 18. From age 40 onward, check it every year. If you have risk factors, check it more often. Free kiosks are available at most pharmacies.
Cholesterol
The AHA recommends your first cholesterol screening between ages 9–11. Adults should recheck every 4–6 years — or more often with known risk factors. Ask for a full lipid panel.
Blood Glucose
A fasting glucose test or HbA1c test screens for prediabetes and diabetes. This is especially important if you carry excess weight or have a family history of diabetes.
CKM Assessment
Ask your doctor specifically about cardiovascular-kidney-metabolic risk if you have high blood pressure, obesity, diabetes, or kidney issues. This is a newer combined risk model that many patients don’t know exists.
Coronary Calcium Scoring
A low-cost CT scan now recommended for adults 40 and older with intermediate risk. It shows actual plaque buildup inside your arteries — before a heart attack happens.
Section 7: Why Heart Disease Does Not Hit Everyone the Same Way
This is a real problem — and it deserves an honest conversation.
Black adults and men experience the highest rates of hypertension-related deaths in the country. The rise in hypertension-related mortality has been tracked across the majority of U.S. counties. It’s not concentrated in one place.
Care quality is also unequal. A major study found that nearly 1 in 4 patients hospitalized for heart attacks still did not receive optimal comprehensive care as recently as 2017. Older adults, women, and Black and Hispanic patients consistently received lower-quality care than others.
Structural barriers make this worse. Food deserts limit access to healthy food. Lack of insurance delays diagnosis. Limited access to cardiologists means fewer people get specialist care when they need it most. Lifestyle advice alone cannot fix a system problem.
But there is one underused resource. Federally Qualified Health Centers (FQHCs) provide sliding-scale cardiac care based on your income. Use HRSA’s free tool at findahealthcenter.hrsa.gov to find one near you.
The AHA also offers free fact sheets specifically on cardiovascular risk in Black, Hispanic, and female populations at heart.org.
Final Words,
Cardiovascular disease now affects nearly half of all U.S. adults. But most risk factors are controllable. Eat whole foods. Move 150 minutes weekly. Monitor your blood pressure, cholesterol, and blood sugar. Work with your doctor.
Heart disease prevention in 2026 starts with a single decision — make it yours.
Half of Americans have cardiovascular disease and most don’t know it. See the AHA’s latest data and 7 simple steps to protect your heart.






