The ‘Normal’ Blood Pressure That Was Quietly Destroying My Arteries for 15 Years (And I Had No Idea)
At 38, my doctor congratulated me on my “healthy” blood pressure of 128/82. Three months later, a cardiac CT scan revealed arterial damage that typically appears in someone 20 years older.
You probably think blood pressure under 140/90 is safe. That’s what I believed too. Your doctor might have said “watch it” and sent you home with no treatment plan. Maybe you assume only readings above 140 are dangerous.
Here’s what nobody told us: blood pressure between 120-139/80-89—called prehypertension or elevated blood pressure—is actively damaging your arteries right now. Not in ten years. Not when it gets higher. Today.
The research is clear. This “borderline” range doubles your risk of heart attack and stroke. It stiffens your arteries, thickens your heart muscle, and damages your kidneys. All silently. All without symptoms.
In this article, you’ll learn exactly what’s happening inside your body at these levels, why it matters more than doctors admit, and the seven evidence-based changes that dropped my blood pressure from 128/82 to 115/74. You’ll also learn how to monitor your BP correctly at home and when to push for medical intervention.

The damage is real. But if you catch it early like I finally did, it’s reversible.
What Doctors Mean When They Say “Just Watch It”
My doctor looked at my 128/82 reading and smiled. “It’s a little high, but nothing to worry about yet.” Those words kept me calm for five years while my arteries quietly deteriorated.
Here’s what he didn’t tell me. Blood pressure between 120-139/80-89 isn’t a gray area. Research shows it doubles your risk of heart attack and stroke compared to readings below 120/80. Nearly half of all heart attacks link back to this “borderline” range.

The real problem? Between 25-50% of adults worldwide sit in this zone. Doctors rarely prescribe medication here. They just say “watch it” and send you home. No diet plan. No exercise guidance. Nothing.
Meanwhile, your arteries are changing. Medical guidelines called this range “not a disease category” for years. But new studies prove otherwise. Every month you spend at 125/82 is a month of measurable damage to your heart and blood vessels.
The Arterial Damage Happening Right Now (That Nobody Talks About)
Your arteries are getting stiffer. Right now. Every heartbeat at 125/82 forces blood through vessels that are slowly losing their stretch. This is called arterial stiffness, and it starts years before you feel anything wrong.
Think of your arteries like rubber bands. Fresh ones snap back easily. Old ones crack and break. Blood pressure in the 120-139 range ages your arteries faster than normal. The damage shows up on a coronary calcium scan—a test that measures hard plaque deposits in your heart arteries. People who spent their twenties and thirties with “borderline” readings show calcium scores of 38% by middle age. Those with normal pressure? Just 15%.
Your heart muscle is also changing. It’s getting thicker and stiffer trying to pump against the resistance. Doctors call this left ventricular hypertrophy. Your kidneys take hits too. So does your brain—prehypertension raises your risk of memory problems later in life.
The worst part? You feel fine. No chest pain. No shortness of breath. Nothing. The damage is completely silent until it becomes a heart attack or stroke. Studies show prehypertension increases your cardiovascular disease risk by 28% compared to optimal blood pressure. Every year you wait is a year of damage you can’t undo.
Why This Happens: The Science Behind ‘Borderline’ Blood Pressure
Your blood pressure has two numbers. The top number (systolic) measures pressure when your heart beats. The bottom number (diastolic) measures pressure when your heart rests between beats. Normal is below 120/80. Elevated is 120-129/80. Prehypertension is 130-139/80-89.
Here’s what happens at 128/82 versus 118/78. Every heartbeat slams blood against your artery walls with extra force. Think of a garden hose. Low pressure keeps it soft and flexible. High pressure makes it hard and brittle over time.
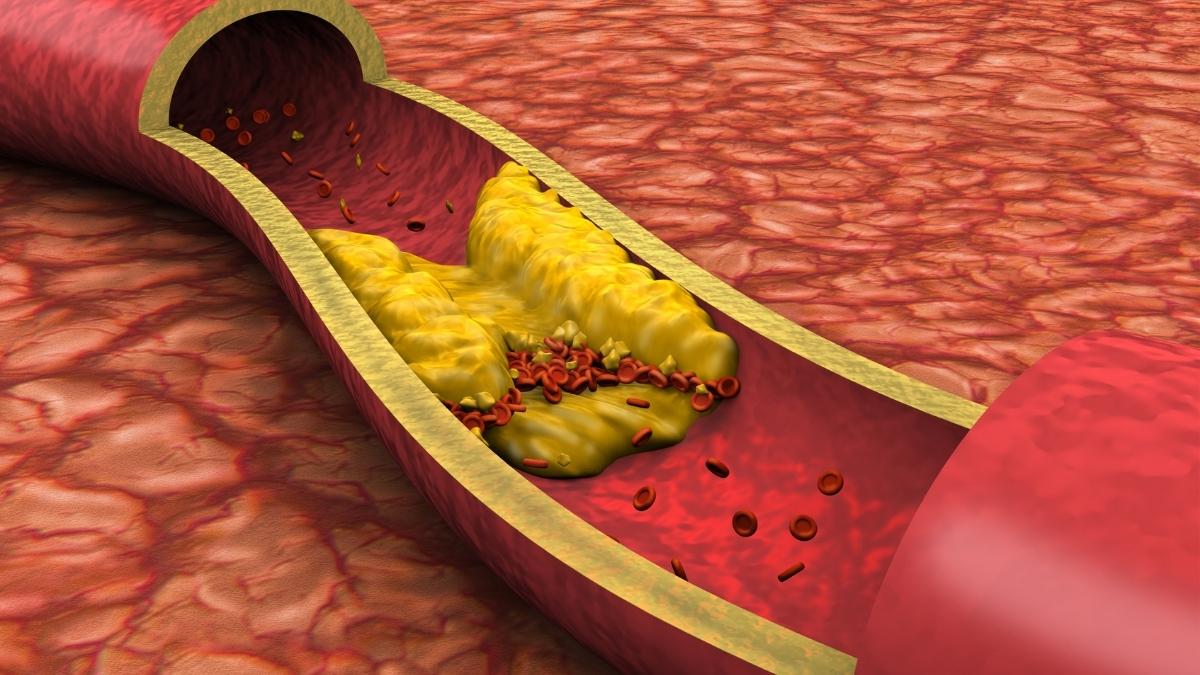
That extra pressure creates microscopic tears in your artery walls. Your body tries to patch these tears with cholesterol and other cells. This builds up as plaque—the same stuff that causes heart attacks. Doctors call this atherosclerosis. It starts small but grows every year you stay in the elevated range.
Most people don’t stay at 125/82 forever. Blood pressure tends to climb as you age. Your forties and fifties are when prehypertension usually becomes full hypertension. Extra weight speeds this up. So does eating too much salt and sitting all day. People with readings of 130-139/85-89 have more than double the cardiovascular disease risk compared to those below 120/80.
The Tests That Finally Revealed My Arterial Age
After three years of “just watching” my 128/82 reading, chest tightness during workouts scared me into action. I paid $99 out-of-pocket for a coronary calcium score CT scan. The test takes ten minutes and measures hard plaque in your heart arteries. My score was 47—moderate risk for someone my age.
But here’s what shocked me. The radiologist said my arterial age looked closer to 57. I was 38. That number made everything real.
Regular doctor visits only check blood pressure and cholesterol. They miss what’s happening inside your arteries. A coronary calcium score shows actual damage. So does a carotid ultrasound, which measures artery wall thickness in your neck (costs $200-300). An echocardiogram checks if your heart muscle is thickening from pumping against resistance.
Most insurance won’t cover these tests unless you have symptoms or high risk factors. Ask your doctor for cardiovascular screening if you’ve had elevated blood pressure for more than two years. The information is worth the cost.
7 Evidence-Based Ways I Reversed the Damage (With Research to Back It)
I didn’t want generic health advice. I wanted proof that specific changes would actually lower my blood pressure. Here’s what worked, backed by real research.
1. The DASH Diet: More Than Just “Eat Healthy”
DASH stands for Dietary Approaches to Stop Hypertension. It’s not a fad diet—it’s a eating pattern proven to drop blood pressure in weeks.
The research is clear. People who followed DASH at 2,300 mg of sodium daily saw their blood pressure fall. Those who cut sodium to 1,500 mg saw even bigger drops. I went straight to 1,500 mg and my systolic pressure dropped 6 points in three weeks.

Here’s what I ate daily: 6-8 servings of whole grains, 4-5 servings of vegetables, 4-5 servings of fruit, 2-3 servings of low-fat dairy, and 6 or fewer servings of lean meat. The key foods are potassium-rich: bananas (420 mg potassium each), white beans, tomatoes, mushrooms, and avocados.
My breakfast: oatmeal with banana and almonds. Lunch: big salad with grilled chicken and beans. Dinner: salmon with roasted sweet potato and broccoli. Snacks: Greek yogurt, apple slices, or a handful of unsalted nuts.
Shopping List Essentials:
- Steel-cut oats and brown rice
- Fresh spinach, kale, and bell peppers
- Bananas, oranges, and berries
- Canned beans (no salt added)
- Plain Greek yogurt
- Skinless chicken breast and salmon
- Unsalted nuts and seeds
2. The Salt Reduction That Actually Worked
I thought I didn’t eat much salt. I was wrong. Most sodium hides in places you’d never guess.
Doctors recommend less than one teaspoon of salt per day (about 2,300 mg of sodium). The ideal target is 1,500 mg. Research shows that switching to potassium-enriched salt instead of regular table salt lowers both blood pressure and heart disease risk.

One slice of bread has 150 mg of sodium. A cup of canned soup? Over 800 mg. Restaurant meals can pack 3,000-4,000 mg in a single dish. I was easily eating 4,500 mg daily before I started tracking.
Hidden Sodium Sources I Cut:
- Deli meat (450 mg per 2 ounces)
- Cheese (200 mg per slice)
- Canned vegetables (300-400 mg per serving)
- Bread and bagels (150-400 mg each)
- Condiments like ketchup and soy sauce (150-1,000 mg per tablespoon)
Practical Swaps That Helped: Fresh chicken instead of deli turkey. Homemade salad dressing instead of bottled. Fresh or frozen vegetables instead of canned. Mrs. Dash and other salt-free seasonings. Potassium chloride salt substitute (tastes almost identical).
Within six weeks of hitting 1,500 mg daily, my blood pressure dropped from 128/82 to 121/78.
3. Exercise: The Type and Amount That Moved My Numbers
I wasn’t sedentary. I walked sometimes. But “sometimes” doesn’t lower blood pressure. Consistency does.
The magic number is 150 minutes per week of moderate exercise like brisk walking, or 75 minutes per week of vigorous exercise like running. That’s just 30 minutes, five days a week. Research shows this can drop systolic blood pressure by 5-8 points.

I started with walking. Nothing fancy. Just 30 minutes around my neighborhood before work. After two months, I added three days of strength training. Recent studies found that wall squats—yes, just holding a squat against a wall—can lower systolic pressure by 8 mmHg.
My Weekly Workout Template:
- Monday: 30-minute brisk walk
- Tuesday: 20 minutes wall squats and bodyweight exercises
- Wednesday: 30-minute walk
- Thursday: 20 minutes strength training
- Friday: 30-minute walk
- Weekend: One longer walk (45-60 minutes) or bike ride
Starting Gradually: Week 1-2: Walk 15 minutes daily. Week 3-4: Increase to 25 minutes. Week 5+: Hit the full 30 minutes. Add strength training only after walking feels easy.
My blood pressure dropped 4 points after the first month of consistent walking.
4. Weight Loss: Even Small Amounts Make a Difference
I needed to lose 35 pounds to hit normal BMI. That felt impossible. Good news: you don’t need to lose it all to see results.
Research shows that losing just 5% of your body weight helps lower blood pressure. For me at 195 pounds, that was less than 10 pounds. Lifestyle changes like diet and exercise can drop systolic pressure by 5-10 points even before major weight loss happens.
I lost 8 pounds in the first two months just from DASH diet and walking. My blood pressure went from 128/82 to 122/79. Another 12 pounds over the next four months brought me to 118/76.
Realistic Goals: Month 1-2: Lose 1-2 pounds per week (8-16 pounds total). Month 3-6: Lose 0.5-1 pound per week (6-12 pounds total). After that: Maintain and reassess.

Crash diets don’t work for blood pressure. You need sustainable changes. I didn’t cut calories drastically—I just ate better quality food in reasonable portions. The weight came off slowly, but my blood pressure improved fast.
5. Stress Management Techniques That Actually Lower BP
I ignored this advice for years. “Relax more” sounded like fluff. But chronic stress keeps your blood pressure elevated all day.
Meditation and deep breathing activate your parasympathetic nervous system, which slows your heart rate and lowers blood pressure. I started with just five minutes of breathing exercises each morning. Breathe in for 4 counts, hold for 4, breathe out for 6. That’s it.

After two weeks, I added 10 minutes of guided meditation using a free app. Within a month, my resting heart rate dropped from 78 to 68 beats per minute. My morning blood pressure readings fell 3-4 points.
Daily Stress Reduction Routine:
- 5 minutes deep breathing right after waking
- 10 minutes meditation before bed
- Two yoga sessions per week (gentle stretching and breathing focus)
- No phone or screens 30 minutes before sleep

Sleep matters too. Research shows 7-9 hours nightly helps regulate blood pressure. I was getting 5-6 hours. Forcing myself to bed by 10:30 PM made a noticeable difference in my morning readings.
6. Alcohol and Caffeine: The Honest Truth
I didn’t want to hear this. I liked my two beers after work and three cups of coffee daily. But both were pushing my numbers up.
Moderate drinking means one drink per day for women, two for men. But research shows any amount of alcohol may raise blood pressure. I cut back to three drinks per week total. My evening blood pressure readings dropped 5 points within two weeks.

Caffeine’s effect is temporary but real. One cup of coffee can spike blood pressure by 5-10 points for 3-4 hours. If you’re drinking coffee all day, your pressure never comes down. I cut from three cups to one morning cup only.
What I Switched To: Morning coffee stayed (couldn’t give that up). Afternoon coffee became decaf green tea. Evening beer became sparkling water with lime. Weekend drinks became occasional, not automatic.

The Transition: Week 1: Cut evening alcohol entirely (hardest week). Week 2: Replace afternoon coffee with herbal tea. Week 3: Try one week completely alcohol-free to see the difference. Week 4: Settle into new pattern (1-3 drinks per week maximum).
Be honest with yourself. If you’re drinking daily, it’s affecting your blood pressure.
7. Supplements That Have Research Support
I tried supplements for months with zero results. Then I learned most don’t work. But a few have real research behind them.
Studies support aged garlic extract, berberine, fish oil (omega-3s), and magnesium for blood pressure reduction. I added these four after three months of diet and exercise changes.

What I Take Daily:
- Aged garlic extract: 600 mg (shown to lower BP by 3-5 points)
- Magnesium glycinate: 400 mg (helps blood vessels relax)
- Fish oil: 2,000 mg EPA/DHA combined (reduces inflammation)
- Berberine: 500 mg twice daily (improves insulin sensitivity and vascular health)
Dosing Guidelines: Start one supplement at a time. Wait two weeks to see effects before adding another. Take with food to avoid stomach upset. Check with your doctor if you’re on blood pressure medication—some supplements can interact.

Which to Prioritize: If you can only afford one, start with magnesium. It’s cheap and well-studied. Add fish oil next if you don’t eat fatty fish twice weekly. Aged garlic and berberine are optional but helpful.
My blood pressure dropped another 3 points after adding these consistently for eight weeks. Combined with lifestyle changes, I went from 128/82 to 115/74.
How to Monitor Your Blood Pressure Correctly at Home
I tracked my blood pressure for six months before realizing I was doing it all wrong. Bad technique can throw your readings off by 10-15 points.
Use an automatic upper arm cuff monitor. Not wrist or finger monitors—they’re less accurate. Get a validated device from validatebp.org. A 2016 study found one-third of home monitors were off by at least 5 points. Omron models consistently score well in Consumer Reports testing. Quality monitors cost $30-$150.
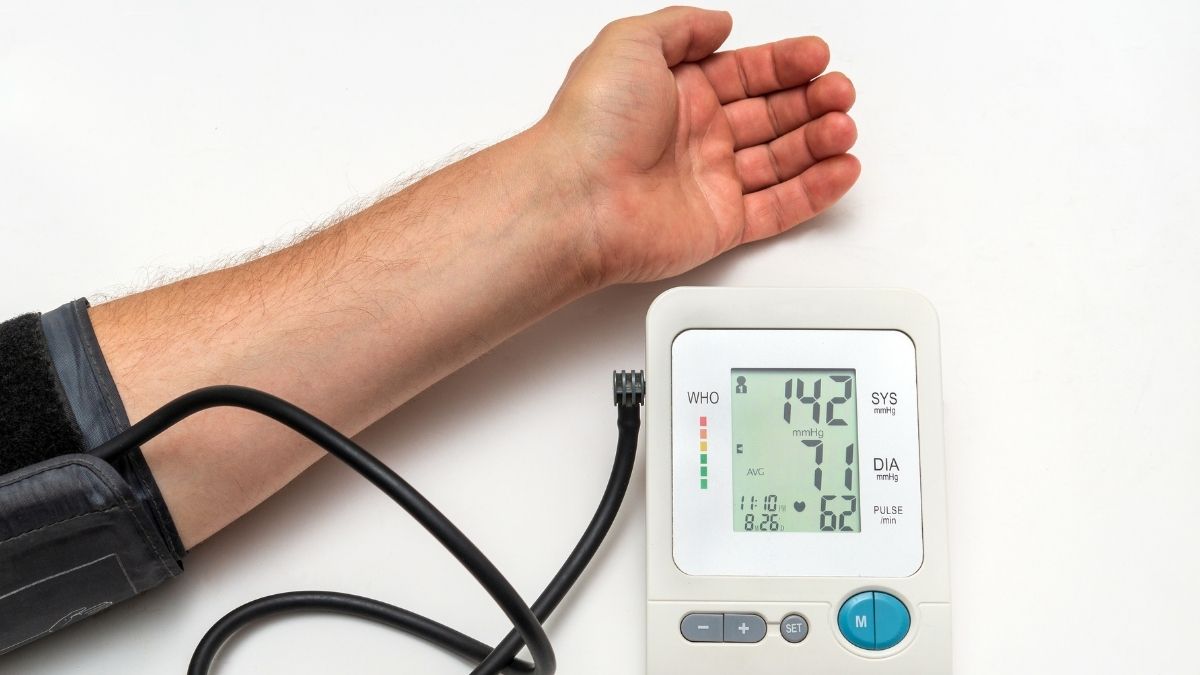
Proper Measurement Technique: Sit quietly for 5 minutes first. Back supported, feet flat on floor, legs uncrossed. Rest your arm on a table at heart level. Don’t talk during the reading. Take two readings 1 minute apart. Average them.
Measure twice daily—morning before medications and evening before dinner. Do this for 5 days, then report the average to your doctor. Skip caffeine, exercise, and smoking for 30 minutes before testing.

Wrong positioning can add 10 points to your systolic reading. An unsupported arm adds another 5-7 points. Getting this right matters.
When to Push for Medical Intervention (And What to Ask For)
I tried lifestyle changes for eight months. They worked. But not everyone sees the same results, and some people need medication sooner.
Current guidelines say patients with blood pressure of 130-139/80-89 should start medication if they have heart disease, diabetes, or kidney disease. Your 10-year cardiovascular risk matters too. If it’s over 10%, medication may help even without other conditions.

Give lifestyle changes 3-6 months. If your blood pressure stays above 130/80 after serious effort with diet, exercise, and weight loss, talk to your doctor about medication. Research shows that preventing one case of hypertension requires treating 4-6 people with medication, or 10 people with intensive lifestyle intervention.
Questions to Ask Your Doctor: What’s my 10-year cardiovascular risk score? Should I get a coronary calcium scan? Am I a candidate for medication given my other risk factors? What’s my target blood pressure?

Red Flags Needing Immediate Attention: Blood pressure over 180/120, severe headache with high BP, chest pain, shortness of breath, vision changes, or difficulty speaking. Don’t wait—call 911.
If your doctor dismisses your concerns about readings consistently in the 120-139 range, get a second opinion. Find a preventive cardiologist who takes prehypertension seriously.
My Blood Pressure Today (And What Happened to My Arterial Age)
Eighteen months after that first coronary calcium scan, I paid for a follow-up. My calcium score stayed at 47—no progression. That’s a win. You can’t reverse calcification, but you can stop it from getting worse.

My blood pressure today averages 115/74. Down from 128/82. That took four months of consistent effort to achieve, and another year to maintain. The first changes showed up in three weeks. Real stability took longer.
I feel different now. I sleep better. My resting heart rate dropped from 78 to 65. No more chest tightness during workouts. I can climb stairs without getting winded.

The Time Commitment: Daily: 10 minutes for BP monitoring and meditation. Weekly: 150 minutes of exercise, meal planning on Sundays. Monthly: About 2 hours total for grocery shopping and prep.
I still check my blood pressure twice weekly. I see my cardiologist annually for follow-up. I can’t undo 15 years of damage, but I stopped it from getting worse at 38 instead of 58.
At the Last,
Blood pressure between 120-139/80-89 isn’t a “gray zone”—it’s actively damaging your arteries, heart, and kidneys right now. The damage is silent. No symptoms. No warning signs. Just years of cumulative harm that leads to heart attacks and strokes.
But here’s the good news: early damage is reversible. DASH diet, sodium reduction, exercise, weight loss, and stress management can drop your blood pressure 10-20 points in 3-6 months. Home monitoring shows you what’s working. Advanced screening reveals the damage before it’s too late.

Do This Week: Check your blood pressure at a pharmacy or buy a validated home monitor. If you’re between 120-139, pick one change from this article and start today. Schedule a coronary calcium scan if you’ve been prehypertensive for years.
Don’t accept “just watch it” from your doctor. Don’t wait until 130 becomes 140, then 160. Act now while the damage is still reversible.
Don’t let borderline blood pressure silently damage your arteries for another year. Start monitoring, start changing, and start protecting your cardiovascular future today.






